What were we obsessed with, invested in, and beset by in 2022? Hazlitt’s writers reflect on the issues, big and small. Keep up with this year’s series here.
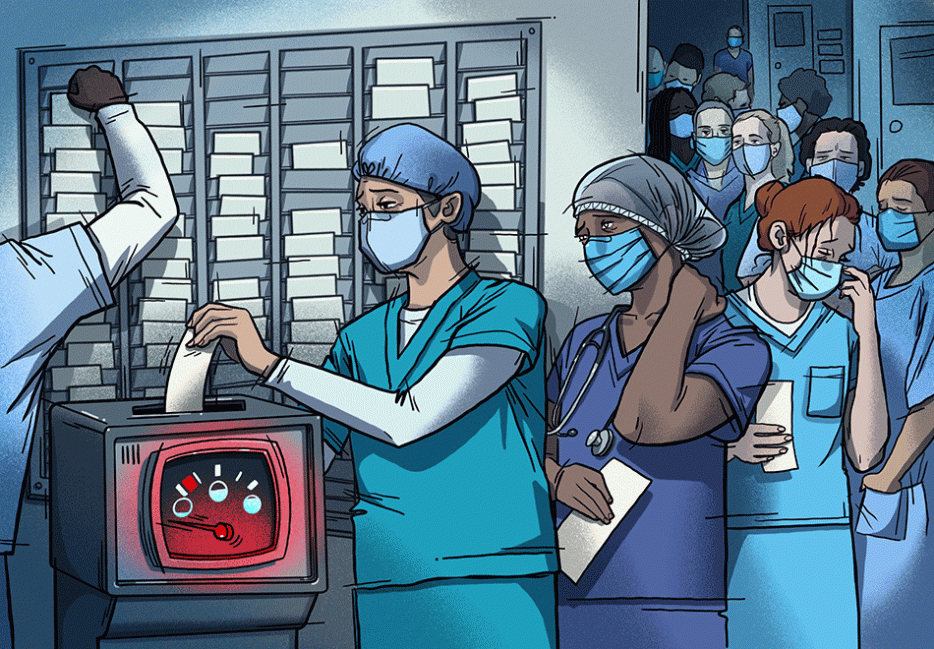
Not long ago, I arrived at the hospital for another night shift in the emergency room. I knew right away it was going to be a bad night. The entire department felt like a wasp’s nest, a flurry of activity in every direction: patients lay on stretchers lining the corridor; others sat in chairs, vomiting into plastic bags; one patient, who had already been there for eight hours, was on his back on the floor moaning loudly, hands covering his face. At the work station nearby, nurses were being hounded by frustrated patients.
One of the nurses sat down next to me, shaking her head and looking utterly defeated.
“I don’t even know,” she said with a blank stare. “Honestly, I just can’t.”
There was suffering all around us. We were trying to keep our heads above water. Short-staffed, no space, and the patients just kept coming.
*
Anyone with even a vague sense of the Canadian news cycle knows that our emergency departments are in crisis. It’s been one of the top stories of the year, making headlines across the country and the world again and again. We hear the story by the numbers: wait times are longer than ever, there aren’t enough beds for the patients that need them, and nursing attrition rates are historically high. They give us a bird’s-eye view, a systems-level narrative about what’s happening. But beyond the statistics and click-worthy headlines, there’s an uncomfortable reality underpinning it all: surrounded by suffering and without any way to help many of the people they’re being asked to treat, frontline health-care workers are being forced to probe the very limits of their own empathy, and the psychological hardship this is causing them is the fulcrum upon which our health-care system is so precariously tipping.
Humans are hardwired to help one another. We develop empathy at a very early age—we even have specialized networks in our brains composed of “mirror neurons” that help us relate to the experiences of others: we wince when we see someone else get hurt, we cringe when we watch someone embarrass themselves, we cry when we see something sad happen even if we’re not directly involved. My daughter isn’t even two years old, but I can already see her beginning to gauge the emotional temperature of the room, tuning into the feelings of the people around her and mirroring what they bring to the table. It seems almost miraculous.
But the human capacity for empathy has its limits. There’s a point at which our empathic brains become overwhelmed, frozen, temporarily incapable of providing a caring response to suffering. It happens in war zones and during famines. It happened in Italy and the United States during the first wave of COVID-19. And it’s currently happening in the Canadian health-care system.
People arrive at the ER every day looking for my help, and the uncomfortable truth is that I’m often so overwhelmed that I struggle to find ways to connect with a lot of them. Sometimes it’s a patient who isn’t having a true emergency and I feel they don’t need to be there; sometimes it’s a patient who is being rude or even violent and I don't want to have to deal with them. But sometimes, sadly, it’s just a perfectly reasonable patient who I don’t have the emotional bandwidth to feel anything for in that moment. I can still do my job, but it feels distinctly unnatural to not care when everything inside you tells you that you probably should. So many of us in health care struggle with this. In our more vulnerable moments we commiserate about it, but too often we struggle in isolation. The firsthand experience of losing your grip on empathy feels a lot like losing a part of your humanity.
*
As a society, we kind of fetishize empathy. Countless self-help podcasts and best-selling books discuss empathy as though it’s a proxy for how good of a person you are. If you can just cultivate empathy you’ll be a better friend, a more attentive lover, and a more understanding parent. From literature to religion to pop culture, we’ve been hearing about the merits of empathy for our entire lives. But under the most trying circumstances, losing one’s empathy is also very human. We all have our limits. There are certain conditions in which humans simply aren’t meant to function. We need to acknowledge this if we’re going to find ways to re-connect. Losing the ability to be empathetic can leave us with a sense of hopelessness and—perhaps worst of all—shame, as though what’s befallen us is somehow our fault when in reality it’s an unavoidable and very human eventuality given the circumstances.
In the ER I can see it on my colleagues’ faces, hear it in their voices, and read it in their postures. I see it in myself, too. It’s rampant, and it’s happening right now. Buzzwords like “burnout” don’t help. They feel vacuous, even flippant. At this point they’re so overused they no longer add anything to the dialogue. We need radically new ways of talking about what it’s like to feel transiently incapable of caring, or we risk pushing more and more amazing, compassionate, skilled, brilliant people away from the health care profession. We’ve already lost so many good people, and if we can’t find a way to make those who are left feel supported during these periods of disconnection, then we’re going to lose a lot more.
Of course I hope our politicians and other stakeholders find a way to work through the logistics of improving our health-care system. But right now my greater hope is that we will find ways to talk about what it’s like to find yourself in a place devoid of empathy, to normalize this experience for those caught in the crosshairs, to humanize what they’re going through and find ways to invite them back into the fold. If we can acknowledge humanity in the most inhuman of circumstances, if we can cultivate empathy for those who have lost touch with it, perhaps we can expand the very borders of empathy itself.